Brain Aneurysm vs. Stroke: What’s the Difference and Why It Matters
Every year, people rush loved ones to the emergency room unsure whether they’re watching a stroke or a brain aneurysm unfold — or whether it even matters. It matters enormously. These two conditions affect the brain in different ways, require different treatments, and carry different risks. Knowing the distinction could one day save a life — possibly your own.
This blog will break both conditions down clearly, explain when they overlap, and tell you exactly what warning signs to act on immediately.
First: What Is a Brain Aneurysm?
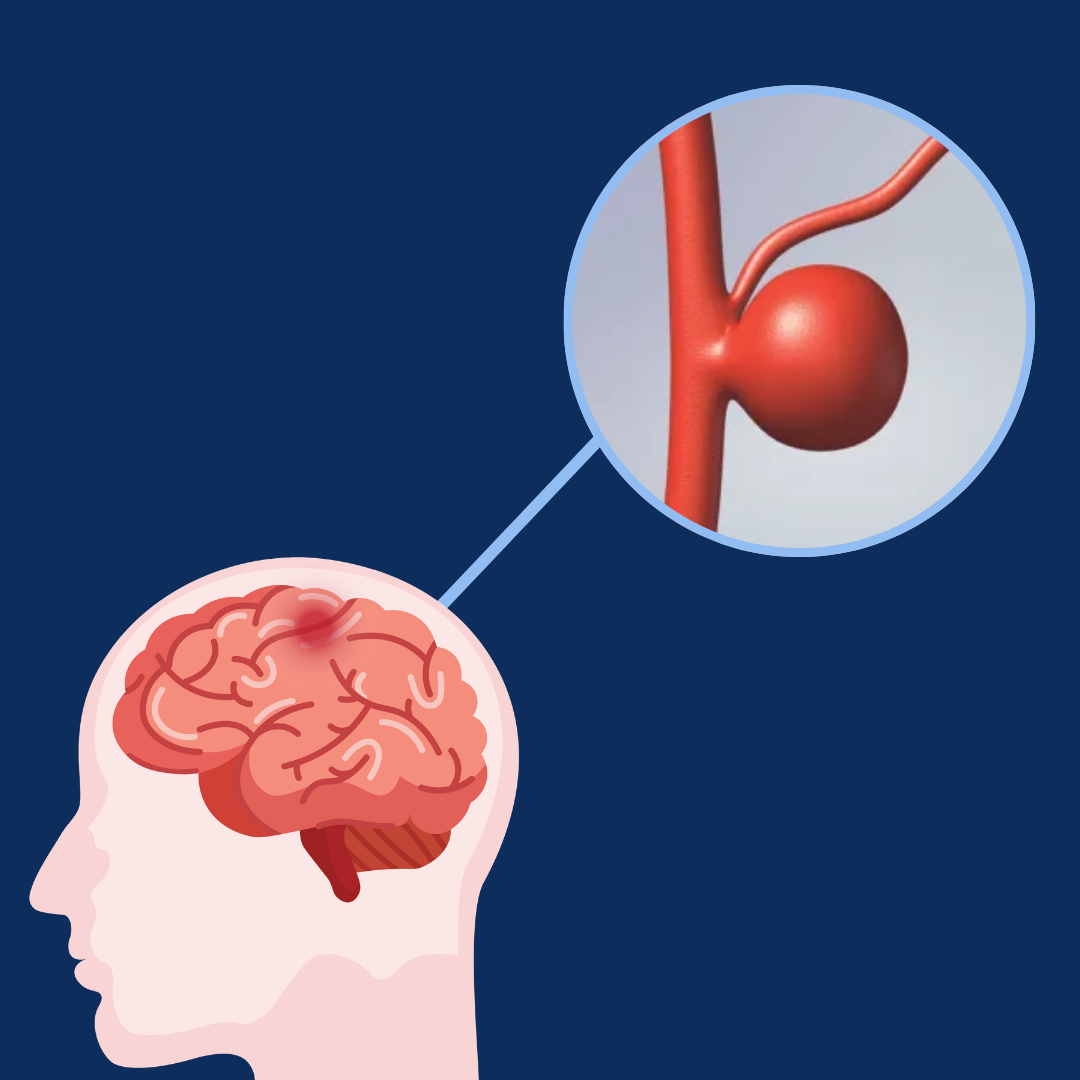
A brain aneurysm is a weak, bulging spot on the wall of an artery in or around the brain, similar to a bubble forming on a worn-out bicycle tire. Most aneurysms sit quietly, causing no symptoms and going completely undetected. Many people live their entire lives with an unruptured aneurysm and never know it.
The danger comes if an aneurysm ruptures. When it bursts, blood floods into the space around the brain, a life-threatening event called a subarachnoid hemorrhage. This is a medical emergency with a mortality rate of around 50%.
Key fact: An aneurysm is a structural weakness in a blood vessel wall. It is not itself a stroke, but a rupture can cause one.
So What Is a Stroke?
A stroke occurs when blood supply to part of the brain is suddenly cut off or when bleeding occurs inside the brain itself. Brain cells begin dying within minutes when they don’t receive oxygen.
There are two main types:
- Ischemic stroke (the most common): a blood clot blocks a blood vessel in the brain, starving brain tissue of oxygen.
- Hemorrhagic stroke: a blood vessel in the brain bursts and bleeds into surrounding brain tissue. This is where strokes and aneurysms overlap most closely.
Key fact: A ruptured brain aneurysm can cause a hemorrhagic stroke — but not all hemorrhagic strokes are caused by aneurysms, and not all aneurysms cause strokes.
Where Do They Overlap?
Here’s where it gets confusing and important. When a brain aneurysm ruptures, blood spills into the subarachnoid space (between the brain and the skull). This event can trigger a hemorrhagic stroke. So in one scenario, an aneurysm rupture and a stroke happen at the same time, one caused by the other.
- Most strokes are ischemic (clot-related) and have nothing to do with aneurysms.
- An unruptured aneurysm does not cause a stroke.
- A hemorrhagic stroke can occur without any aneurysm, from high blood pressure damaging vessel walls, for example.
The practical takeaway: these are distinct conditions that require different responses and different long-term care.
Symptoms: How to Tell Them Apart

- A sudden, severe headache — often described as the worst headache of your life
- Neck stiffness or pain
- Nausea and vomiting
- Sensitivity to light
- Brief loss of consciousness
- Blurred or double vision

- Face drooping on one side
- Arm weakness — can you raise both arms equally?
- Speech difficulty — slurred, strange, or absent
- Time to call 911 immediately
Important: The hallmark of an aneurysm rupture is the thunderclap headache — a sudden, explosive headache that peaks within seconds. Strokes more commonly present with facial drooping, arm weakness, and speech problems. If you see either set of symptoms, treat it as an emergency.
How Each Is Diagnosed and Treated
Brain aneurysm: Unruptured aneurysms are often found incidentally via MRI or CT scan. A ruptured aneurysm is diagnosed via CT scan or lumbar puncture. Treatment options include surgical clipping (a clip placed at the aneurysm’s base to stop blood flow) or endovascular coiling (a minimally invasive procedure to fill the aneurysm with tiny coils).
Stroke: Ischemic strokes are often treated with tPA (a clot-busting drug) if administered quickly, or mechanical thrombectomy to remove the clot. Hemorrhagic strokes require stopping the bleeding and managing pressure in the brain, and if caused by an aneurysm, the aneurysm itself must also be treated.
Who Is at Risk?
Both conditions share some risk factors, but differ in important ways.

- Family history of brain aneurysms
- Being female (women are more commonly affected)
- High blood pressure
- Smoking
- Certain inherited conditions (such as polycystic kidney disease)

- High blood pressure (the leading risk factor)
- Atrial fibrillation and other heart conditions
- Diabetes
- High cholesterol
- Smoking and physical inactivity
The Bottom Line
Brain aneurysms and strokes are not the same thing, but they can intersect in dangerous ways. Understanding the difference means you’ll know what to watch for, when to act, and what questions to ask a doctor.
If someone near you experiences a sudden severe headache unlike anything they’ve felt before, or shows signs of facial drooping, arm weakness, or speech difficulty — call 911 immediately. Don’t wait. Don’t drive yourself.
Know Your Risk. Share This Post.
Brain aneurysms affect an estimated 6.8 million people in the United States, most of whom don’t know it. Share this article with someone you love and encourage them to talk to their doctor if they have a family history or any of the risk factors above.
Visit bafound.org to learn more about brain aneurysm screening, support resources, and how to get involved.


 Brain Aneurysm Foundation
Brain Aneurysm Foundation