Kelly’s Story

Kelly Messmer of Indiana with her husband and two sons.
On my fourth birthday, my mother suddenly placed her hands on her head while we were stopped at a traffic light. We had just picked up my birthday cake, planning to celebrate later that day. But that party never happened.

I was in the back seat, a family friend in the passenger seat. Not understanding what was happening, my mom’s friend quickly put the car in park. My mother, just 34 years old, never regained consciousness. Crawling over her in the car was the last time I saw her awake. The next day, she passed away from a cerebral aneurysm. For days, she had been complaining of severe headaches. My dad had planned to take her to the hospital after my birthday—but it was too late.
Later, I was taken to my grandparents’ house, where I met up with my older brother. I remember my dad sitting us down on a bed in a quiet bedroom. He told us, with a calmness I couldn’t fully understand, that our mom was never coming back and that she had died from a cerebral aneurysm. I put my head down and cried, though at four, I didn’t truly grasp the enormity of what had just happened. Later, I went and played with my birthday toys, a small attempt to return to normal, even though the world I knew had changed forever.
That day introduced me to loss, fear, and the fragile nature of life. It was the beginning of a story that would follow me for decades, a story of a family shadowed by Polycystic Kidney Disease and aneurysms, a story that would one day become my own.
Growing up, I knew that polycystic kidney disease (PKD) and brain aneurysms ran in my family. My maternal grandmother and uncle both had PKD and an aneurysm that ruptured, but were clipped and not fatal like my mother’s. My uncle had undergone 2 kidney transplants and had some paralysis of his hand and leg due to his ruptured aneurysm. My aunt also had PKD, and she passed away on dialysis at 67. PKD was traced back to my maternal grandmother’s father’s side.
At 20, I experienced a severe headache while on a trip, which landed me in the hospital with dangerously high blood pressure. Why would a 20-year-old have hypertension? That hospital stay led to my diagnosis of PKD—a non-curable disease.
Since my diagnosis, regular kidney scans have been crucial. I’ve battled kidney stones, anemia, and cysts on my liver. During my first pregnancy, I developed high blood pressure, which put strain on my kidneys. Wanting to protect my health for my second child, I went through four rounds of IVF and chose a gestational carrier to bring my second son into the world.

Alongside kidney monitoring, I’ve undergone regular cerebral MRIs every 2–3 years since I was 20 to screen for aneurysms. Each time I entered that MRI tube, I thought about my mother and others—like a high school friend of mine—who never had the chance to receive this kind of preventive care. I’ve always felt incredibly lucky that if an aneurysm were found, I’d have the opportunity to fight it.
Then, the day before Thanksgiving in 2024, by the Grace of God, I got the call that changed everything. At 42 years old, my MRI had detected a possible aneurysm. A follow-up CT scan and cerebral angiogram confirmed what I had feared—but also validated the importance of being proactive.
A cerebral angiogram is a frightening but necessary procedure. My incredible surgeon accessed my femoral vein and threaded a catheter through my blood vessels up to my brain, where contrast dye was injected to capture detailed images. The sensations were bizarre, the procedure intense. I had to stay awake under conscious sedation, following breathing instructions carefully. The results? A 4 mm aneurysm—small, but significant. Surgery was recommended, given my family history.
June 24, 2025, is a day I will never forget. That morning, I walked into Northwestern Hospital for a craniotomy to clip my brain aneurysm, something my mom never had the chance to do. I carried fear, prayers, and a quiet hope that I could write a different ending.

The surgery itself felt overwhelming. I worried about complications, strokes, seizures, and even the emotional weight of having part of my head shaved. Yet beneath the fear was an unexpected sense of peace, a steady confidence that this was the step I needed to take to protect my life and my family.
Next came the team, the people who would be with me through one of the most critical moments of my life. About eight to ten individuals introduced themselves. The Chief Resident explained the procedure, followed by the anesthesiology team, who reviewed the anesthesia plan and addressed risks and concerns. I was connected to monitors tracking my heart rate, blood pressure, oxygen levels, and breathing. Everything felt very real.
I made my final FaceTime calls to family and then said goodbye to my husband. Tears streamed down my face as I left the room. The team walked beside me as I was wheeled to the operating room. Once inside, I began to shake from nerves and the cold. A nurse wrapped me in a warm blanket, a small kindness that meant everything.
As I lay on the gurney, I watched the team move efficiently. A medical student on an eight-week rotation noticed my emotions and came over to talk. She asked about my kids and my family, and I asked about her life and career aspirations. That brief conversation was grounding, comforting, and deeply human. I will always be grateful for her. Just before anesthesia, my surgeon came in, shook my hand, and told me I would be okay.
When I was first diagnosed, I immediately came to the BAF for resources like stories and support. The BAF support group has been absolutely amazing, and I was able to ask questions, and within minutes, my questions were answered. I am very grateful for the BAF.
When I woke up, the first words I heard from him were simple: “It’s time to walk.” And so I did.
I was wheeled back to my room for monitoring and rest. My pain was managed with Tylenol, along with medications for nausea and seizure prevention. That first day, I barely ate and did get sick. A few hours later, I was finally able to see my husband, and that moment alone brought comfort. My head was wrapped, my face swollen, and my eyes black and blue. I was too afraid to touch my head, though I was desperately curious about how much hair had been shaved.
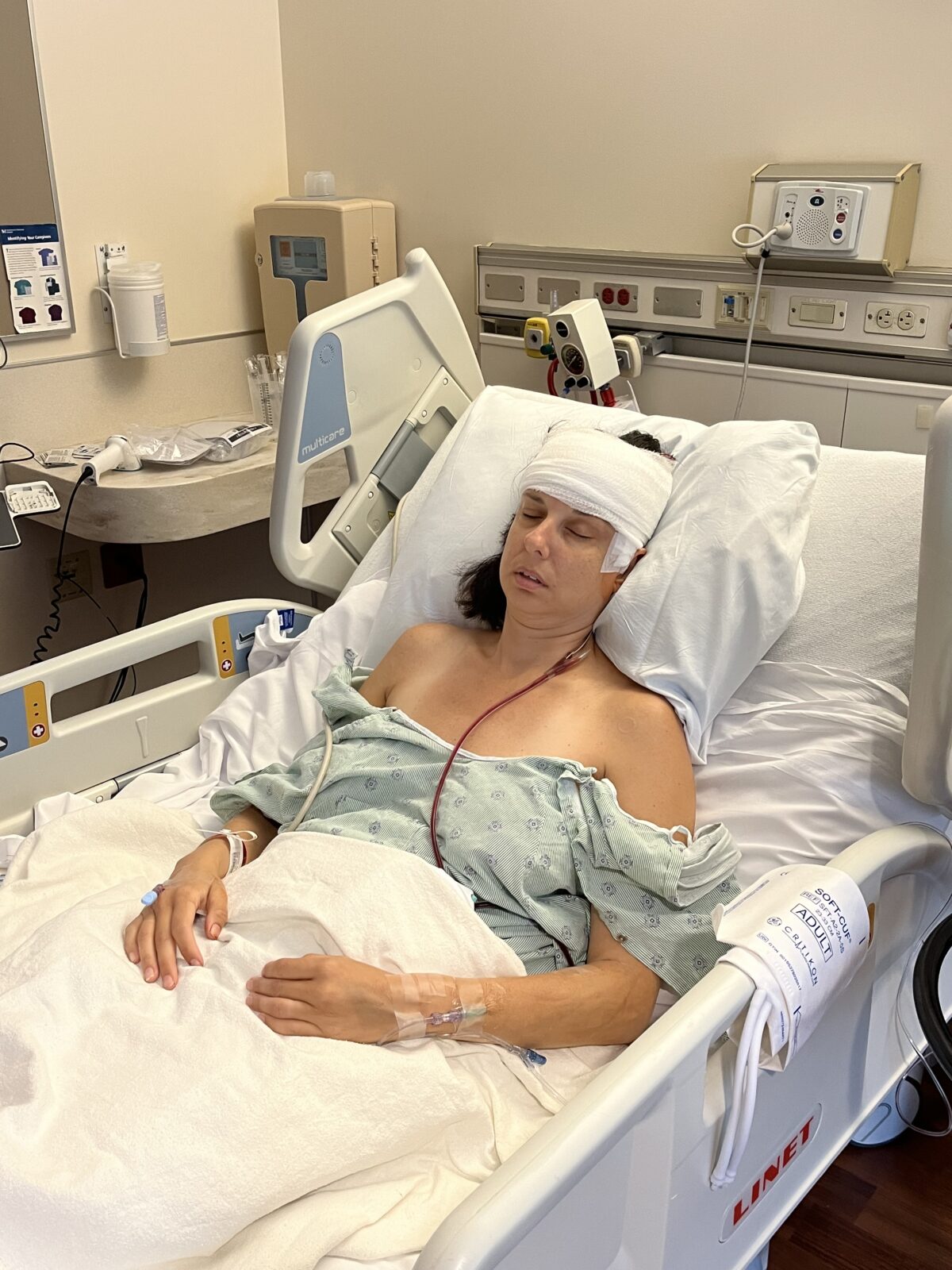
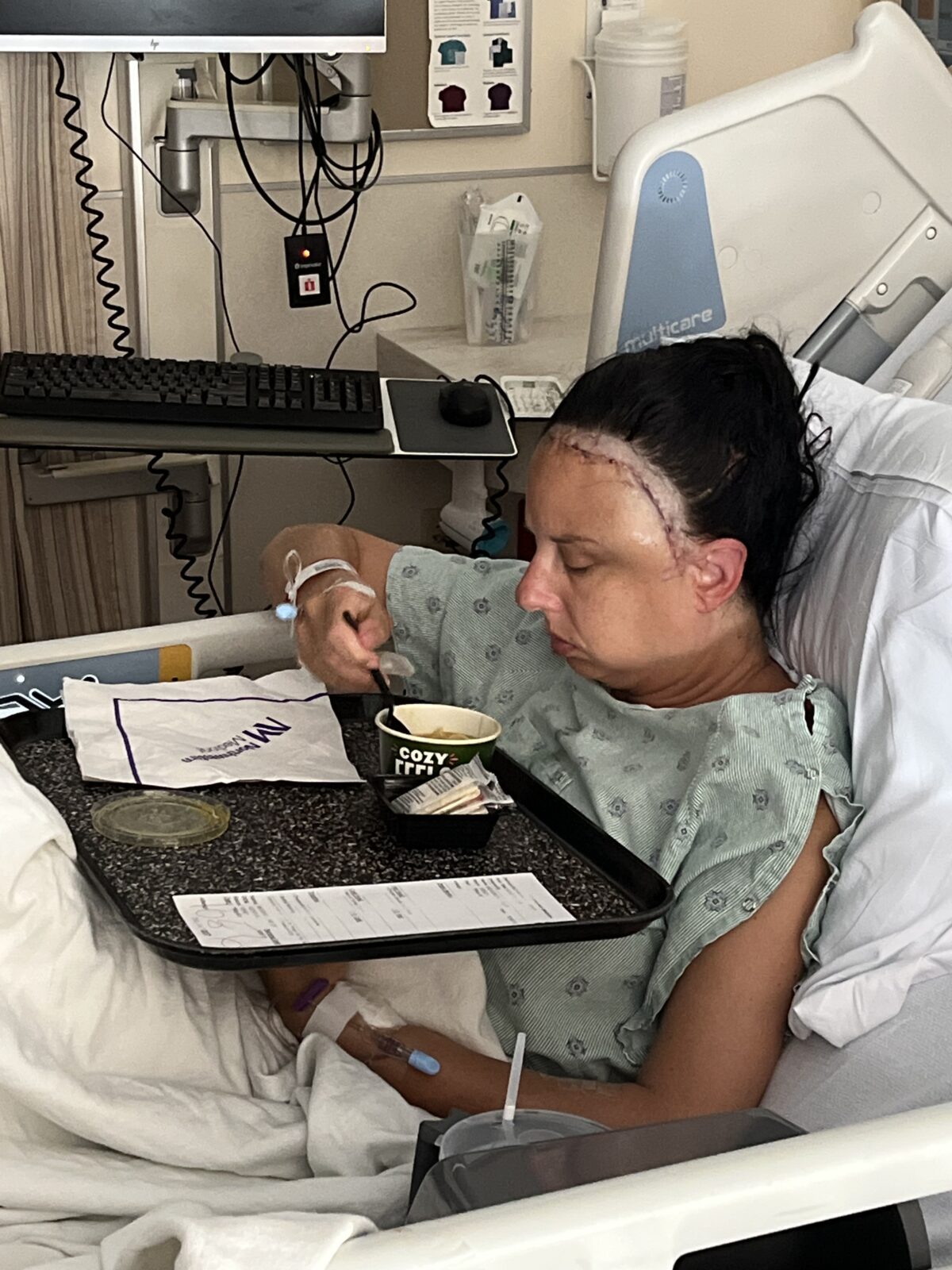

The first week at home was quiet and slow. I took my first shower with help washing my hair. I walked small laps upstairs and then returned to bed. I saw my oldest son but waited about five days before seeing my youngest. Eating was difficult. Opening my mouth and chewing hurt. I stayed diligent with my medications, though I looked forward to slowly reducing Tylenol.
By the second week, my face was still puffy and bruised, but my hair began to poke through along the incision line. I walked short distances in the backyard, then a tenth of a mile down the road and back, followed by rest. By the end of week three, the bruising had faded, my hair had grown a bit more, and my head became incredibly itchy from regrowth, a sensation that lasted for months.
I eventually worked my way up to walking three miles. Looking back, I am not sure if that was too much, but I was determined to reclaim movement. I listened to my body, stopping whenever my heart rate climbed too high. Every step reminded me that I had been given a second chance at life, one my mother never had. I still took daily afternoon naps, honoring what my body needed.

Three months after my brain aneurysm surgery, I found myself reflecting on just how much had changed, and how much I had to be grateful for.
Recovery became a journey of small victories. Walking laps around the neighborhood, regaining strength, and slowly returning to the routines that brought me joy, all reminded me of the second chance I had been given. Every step, every breath, every moment with my family became a gift.
This journey reinforced the lessons I had learned throughout my life, that faith sustains us in times of fear, resilience is built one step at a time, and that community and love are as essential as any medical intervention.
Living with gratitude also deepened my commitment to raising awareness about PKD and brain aneurysms. Early detection saved my life, and I hope sharing my story encourages others to prioritize regular checkups, scans, and proactive care.
Most of all, this experience reminded me to live fully and intentionally. Life is fragile, unpredictable, and infinitely precious. Even under the shadow of a chronic disease, and after facing a life-threatening aneurysm, I am here, stronger, more aware, and profoundly thankful.
It’s surreal to realize I was around my youngest son’s age when my mother had her aneurysm. But unlike her, I have the gift of early detection. I’m now part of a PKD study at the University of Maryland and newly enrolled in a study focused on PKD patients with aneurysms. My greatest hope and prayer is for a cure—because my boys have a 50/50 chance of inheriting this disease.
Through it all, one truth remains clear: every scan is more than a test. Every scan carries hope, hope that can guide us, protect us, and sometimes even save our lives.


 Brain Aneurysm Foundation
Brain Aneurysm Foundation